Thumb base arthritis is a common cause of pain at the base of the thumb. It can affect grip, pinch strength, opening jars, writing, using tools, and day-to-day hand function.
At Peak Orthopaedics, thumb carpometacarpal (CMC) joint replacement is now available locally in New Plymouth for selected patients with thumb base arthritis.
This provides another surgical option alongside non-operative treatment, trapeziectomy, and fusion. The aim is to reduce pain while preserving thumb movement and function where appropriate.
What is thumb CMC arthritis?
The thumb CMC joint is the joint at the base of the thumb, where the thumb metacarpal meets the wrist. It allows the thumb to move in multiple directions, including pinch and opposition.
With arthritis, the joint surface becomes worn. This can lead to pain, stiffness, weakness, swelling, and difficulty with activities that require gripping or pinching.
Symptoms may include:
Pain at the base of the thumb
Difficulty opening jars or bottles
Pain with gripping, pinching, writing, or using tools
Weakness of pinch grip
Swelling or prominence around the thumb base
Reduced thumb movement or function
Treatment options
Not every patient with thumb base arthritis needs surgery. Treatment depends on symptoms, x-ray findings, hand function, activity level, and patient preference.
Non-operative options may include:
Activity modification
Splints or braces
Hand therapy
Anti-inflammatory medication where appropriate
Corticosteroid injection
Surgical options may include:
Trapeziectomy
Thumb CMC fusion
Thumb CMC joint replacement
Each option has advantages and limitations. The most suitable option depends on the individual patient.
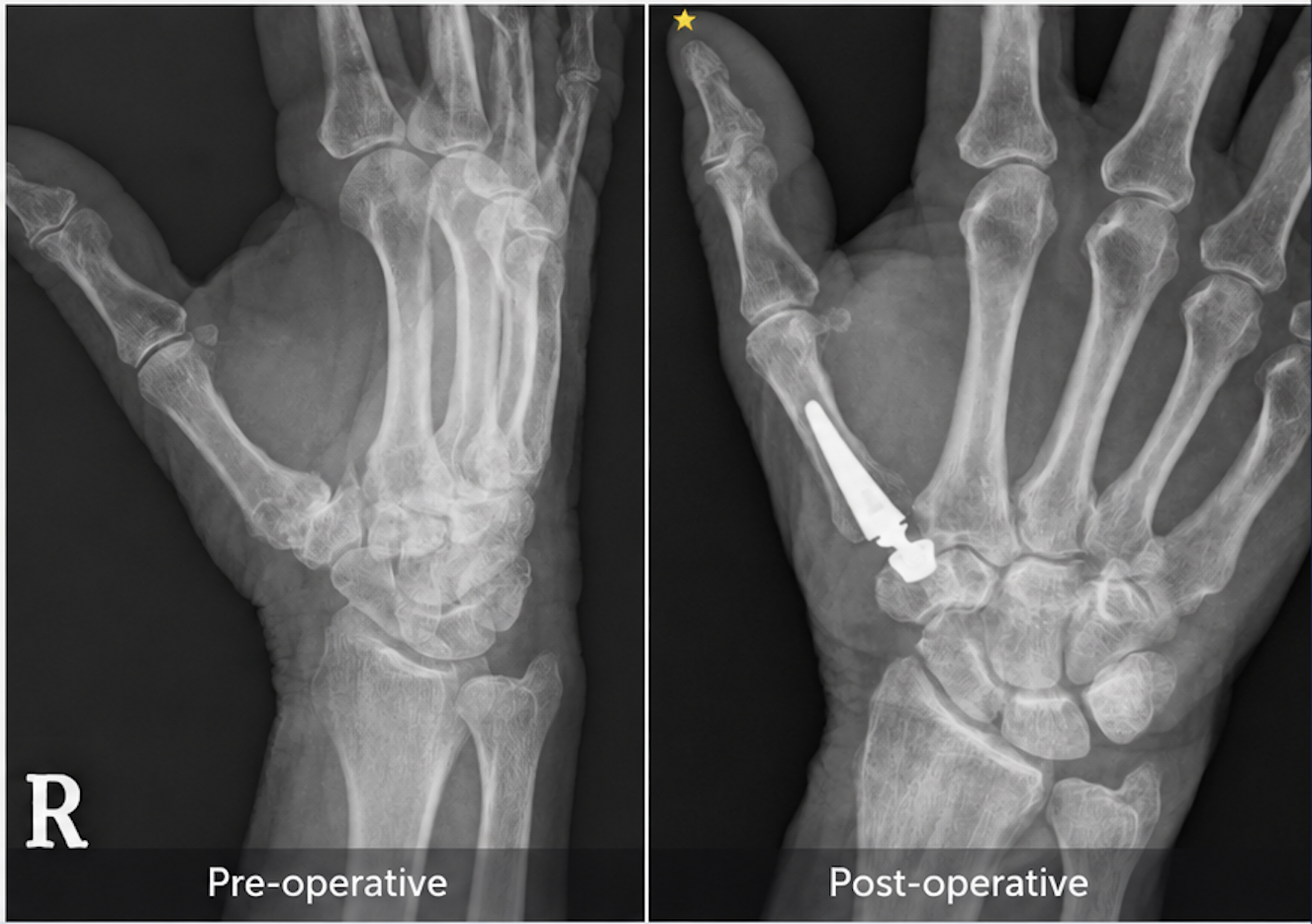
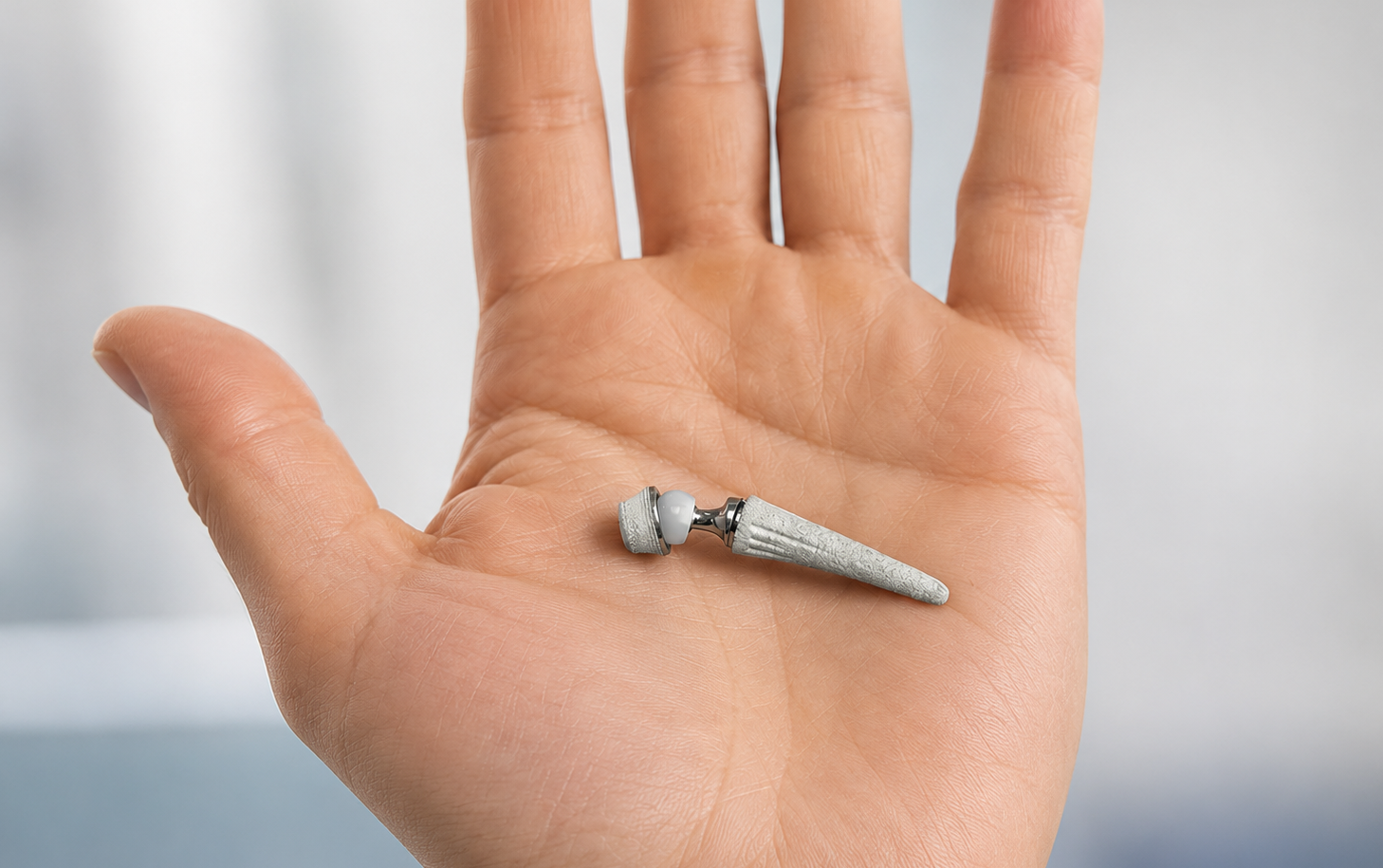
What is thumb CMC joint replacement?
Thumb CMC joint replacement involves replacing the worn joint surface at the base of the thumb with an artificial joint.
The aim is to:
Reduce pain
Preserve thumb motion
Improve function
Maintain thumb length and mechanics where possible
Support return to everyday activities
It is not suitable for everyone, but in carefully selected patients it can be a very useful option.
Who may be suitable?
Thumb CMC joint replacement may be considered for selected patients with:
Painful thumb base arthritis
Symptoms affecting grip, pinch, work, hobbies, or daily activities
Failure of non-operative treatment
Good bone quality and suitable joint anatomy
A desire to maintain thumb movement and function
A full assessment, examination, and x-rays are required to decide whether joint replacement is appropriate.
Why patient selection matters
“I have taken a cautious and selective approach to introducing thumb CMC joint replacement locally in New Plymouth.
Careful patient selection, surgical technique, and close follow-up are important. Outcomes to date have been very encouraging, particularly in terms of pain relief, function, and recovery in suitable patients.”
Recovery after thumb CMC joint replacement
Recovery varies between patients and depends on the procedure performed, bone quality, soft tissue condition, and individual rehabilitation progress.
In general, recovery involves:
A protective dressing and splint initially
Wound review and early follow-up
Gradual return of thumb and hand movement from 2 to 3 weeks post surgery
Hand therapy input
Progressive strengthening once healing allows
Most patients should expect a period of protection followed by gradual return to normal hand use. Heavy gripping, forceful pinch, and high-load activity are usually delayed until the joint has had time to settle.
Specific recovery advice will be provided after assessment and surgery.
Referral and assessment
Francis Ting is happy to review patients with thumb base arthritis for assessment and discussion regarding operative versus non-operative management.
This includes discussion of whether thumb CMC joint replacement, trapeziectomy, fusion, injection, splinting, or hand therapy is the most appropriate option.
Referrals are welcome from GPs, physiotherapists, hand therapists, and other health professionals.